In today’s evolving healthcare environment, rising payer complexity, increased regulatory scrutiny, and tightening margins demand a robust, data-driven Revenue Cycle Management (RCM) system. According to current industry research, effective RCM can prevent revenue leakage and reclaim up to 10% or even more of lost revenues.
At Panacea Pro Corporation, we serve as a critical extension of your practice and RCM team—ensuring every dollar earned is a dollar collected.
We specialize in end-to-end RCM services, helping providers increase clean claim rates, accelerate reimbursements, reduce denials, and gain real-time insight; into financial performance.
In today’s evolving healthcare environment, rising payer complexity, increased regulatory scrutiny, and tightening margins demand a robust, data-driven Revenue Cycle Management (RCM) system. According to current industry research, effective RCM can prevent revenue leakage and reclaim up to 10% or even more of lost revenues. At Panacea Pro Corporation, we serve as a critical extension of your practice and RCM team—ensuring every dollar earned is a dollar collected.
We specialize in end-to-end RCM services, helping providers increase clean claim rates, accelerate reimbursements, reduce denials, and gain real-time insight into financial performance.
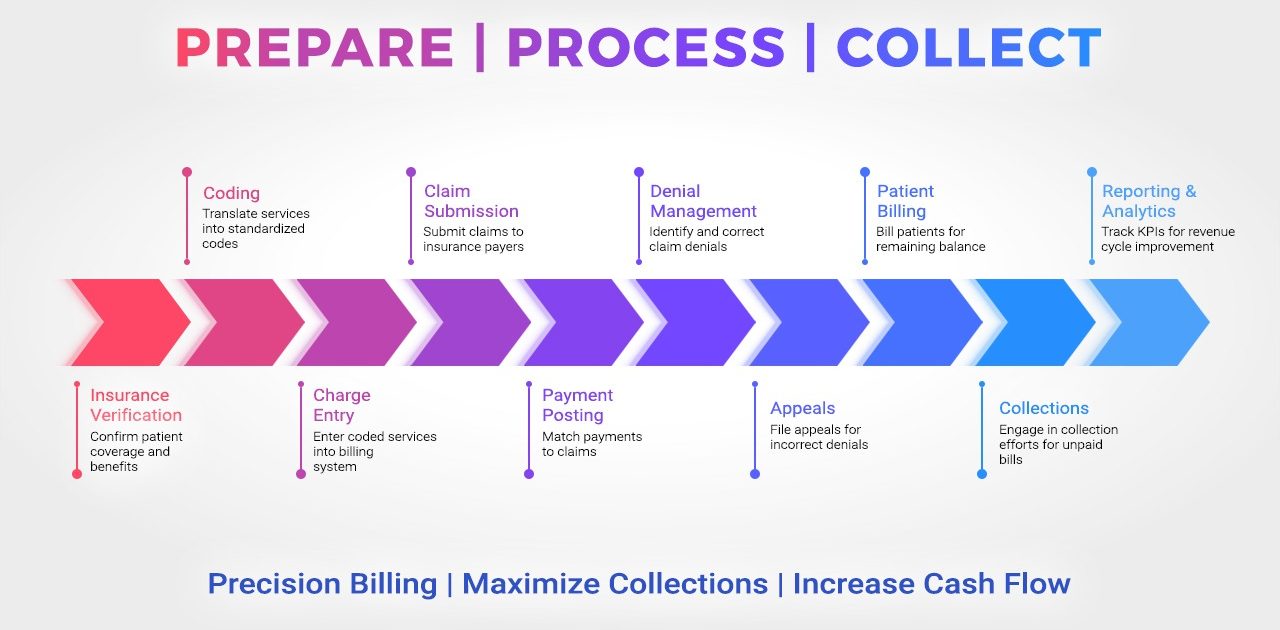
We offer a scalable and HIPAA-compliant RCM solution, fully customisable based on your practice size, speciality, and payer mix.
Verify patient insurance eligibility in real-time to prevent claim denial.Improve your medical billing accuracy and speed with automated eligibility checks.
Ensure clean claim submission with accurate patient demographic data.Eliminate billing errors through meticulous data entry and verification.
Capture every service detail for precise charge entry and faster reimbursements. Optimize your medical billing workflow with completely error-free charge capture.
Submit electronic claims daily to accelerate payment cycles. Reduce claim backlogs with efficient EDI and healthcare RCM automation.
Handle multi-level insurance billing seamlessly for faster reimbursements.Maximise collections through efficient claim routing and follow-up.
Monitor every claim’s status in real time with advanced RCM tools. Resolve issues quickly to speed up the adjudication process.
Post insurance and patient payments accurately to maintain clean financials. Simplify reconciliation to ensure complete revenue transparency.
Analyze denials to identify patterns and prevent future rejections.Strengthen your appeals process for faster claim recovery.
Proactively follow up on unpaid claims and patient balances. Reduce A/R days with consistent insurance & patient communication.
Send automated patient statements and gentle payment reminders.Boost patient collections without compromising satisfaction.
Get bi-weekly or monthly RCM reports with financial insights. Make smarter decisions with transparent operational analytics.
We follow up on unpaid claims after 20 days—not the industry-standard 30+ days.
Using automation and expert auditing.
Ensuring fewer write-offs and quicker payments.
We’re equipped for both electronic and paper claims across Medicare, Medicaid, HMOs, PPOs, Workers’ Compensation, Personal Injury, and self-pay patients.
We assist in identifying optimal place-of-service codes, proper use of modifier combinations, and maximize procedural reimbursements under payer guidelines. Each Explanation of Benefits (EOB) is carefully reviewed. We act immediately on underpaid or denied claims and submit appeals when warranted. We also manage secondary claims promptly after primary payer EOBs to ensure patients are not overburdened.
Aged A/R follow-up on accounts > 30 days
Appeal preparation and submission for denied or low-pay claims
Soft collections: courtesy calls, letters, and payment reminders
Support for peer reviews, reconsideration requests, and medical dispute resolution
Our reports shows clear insight into practice health, empowering informed financial decisions.
Schedule a Meeting for a complimentary RCM health check and see how we can help your practice thrive.
We are committed to excellence in service delivery, ensuring quality, accuracy, and security at every stage.
We are committed to excellence in service delivery, ensuring quality, accuracy, and security at every stage.
Schedule a Call for a complimentary RCM health check and see how we can help your practice thrive.
© 2025 Panacea Pro Corporation. All Rights Reserved